Emergency Conditions in Primary Healthcare
📑 40 slides
👁 80 views
📅 2/9/2026
Introduction to Emergency Conditions
Overview of common emergencies in primary healthcare

2
Snake Bites: General Overview
- Globally, 5 million snake bites occur annually
- Venomous snakes cause 138,000 deaths yearly
- Key symptoms: pain, swelling, necrosis

3
Types of Snake Venom
- Neurotoxic: affects nervous system (cobras, kraits)
- Hemotoxic: damages blood vessels (vipers)
- Cytotoxic: tissue destruction (some vipers)

4
Snake Bite First Aid
- Immobilize limb and keep below heart level
- Remove constrictive items (rings, watches)
- Avoid cutting, sucking, or tourniquets
5
Antivenom Administration
- Give only for systemic envenomation signs
- Start with 10 vials for severe envenomation
- Monitor for anaphylaxis (occurs in 10% cases)
6
Scorpion Stings Overview
- 3000+ species, 50 dangerous to humans
- Most deaths occur in children under 10
- Primary toxins: neurotoxins affecting Na+ channels

7
Scorpion Sting Symptoms
- Local: intense pain, swelling, paresthesia
- Systemic: hypertension, tachycardia
- Severe: pulmonary edema, cardiogenic shock

8
Scorpion Sting Management
- Local wound care and analgesia
- Prazosin for autonomic storm symptoms
- Antivenom for severe systemic reactions
9
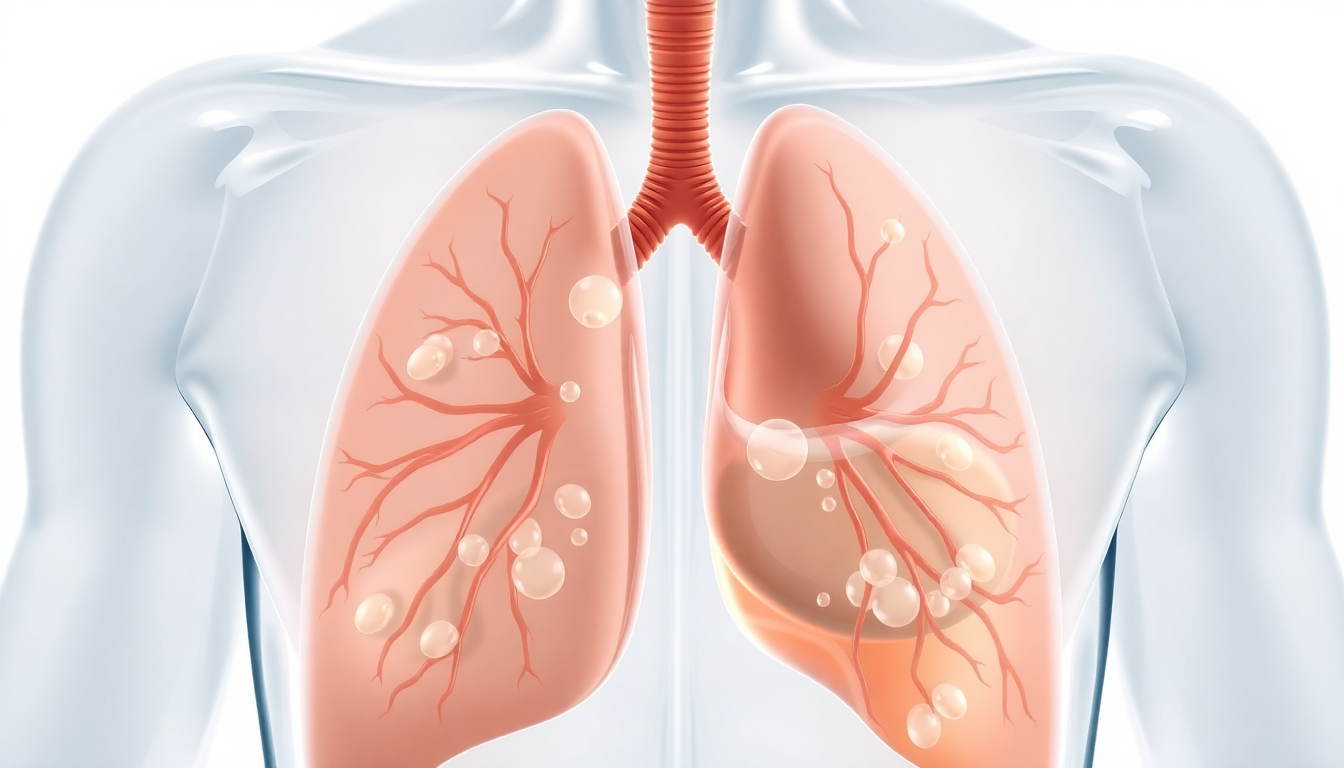
Pleural Effusion: Definition
- Accumulation of fluid in pleural space
- Transudate vs exudate (Light's criteria)
- Common causes: CHF, pneumonia, malignancy
10
Pleural Effusion Diagnosis
- CXR: blunted costophrenic angle (200ml+)
- Ultrasound: most sensitive bedside tool
- Diagnostic thoracentesis for fluid analysis
11
Pleural Effusion Management
- Treat underlying cause (diuretics for CHF)
- Therapeutic thoracentesis for dyspnea
- Chest tube for empyema (>7.2 pH)
12
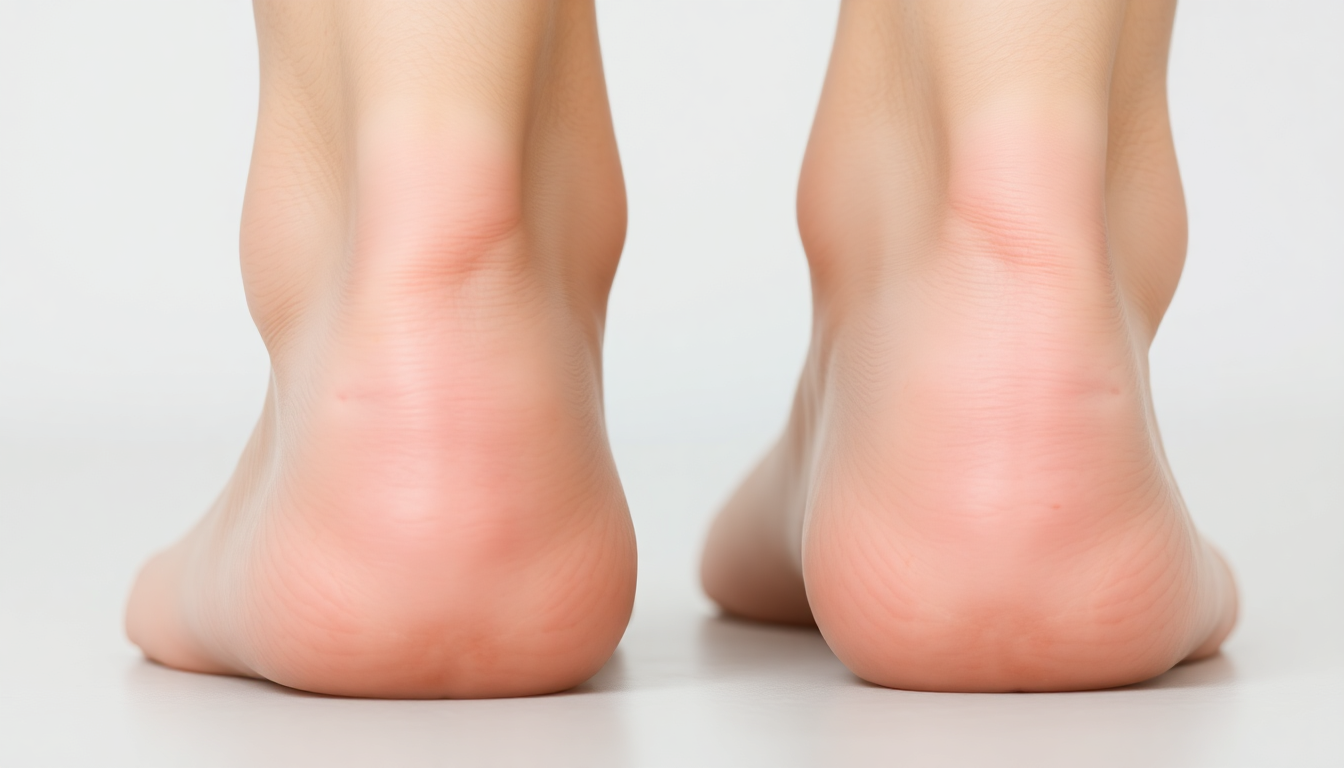
Lower Limb Edema Causes
- Venous insufficiency (most common)
- DVT, CHF, renal failure, liver cirrhosis
- Lymphatic obstruction (filariasis)
13
Lower Limb Edema Evaluation
- Unilateral vs bilateral presentation
- Check for warmth, redness (DVT signs)
- Assess JVP, heart/lung exam for CHF
14
Lower Limb Edema Treatment
- Compression stockings for venous disease
- Diuretics for cardiogenic edema
- LMWH for DVT (after confirmation)
15
Atrial Fibrillation Basics
- Most common sustained arrhythmia
- Prevalence: 3% adults >20 years
- Key risks: stroke (5-fold increase)

16
AFib Classification
- Paroxysmal (<7 days, self-terminating)
- Persistent (>7 days, needs intervention)
- Permanent (accepted as chronic)

17
AFib Acute Management
- Rate control (beta-blockers, CCBs)
- Rhythm control (cardioversion)
- Anticoagulation based on CHA2DS2-VASc
18
AFib Stroke Prevention
- Warfarin (INR 2-3) or DOACs
- LAA occlusion for high-bleeding risk
- Avoid aspirin monotherapy
19
Chest Pain Differential
- Cardiac: ACS, pericarditis, dissection
- Pulmonary: PE, pneumothorax
- GI: GERD, esophageal spasm

20
ACS Recognition
- Typical pain: substernal, radiating
- Atypical presentations in women, diabetics
- ECG changes (ST elevation/depression)
21
PE Diagnostic Approach
- Wells score to assess probability
- D-dimer for low probability cases
- CTPA for high probability or +D-dimer
22
Aortic Dissection Signs
- Tearing pain radiating to back
- Pulse deficits (30% cases)
- CXR: widened mediastinum (60%)

23
Diabetic Ketoacidosis
- Defined by: glucose >250, pH <7.3, ketones
- Mortality: 1-5% in developed countries
- Precipitants: infection, non-compliance
24
DKA Pathophysiology
- Absolute insulin deficiency
- Counterregulatory hormone excess
- Resultant hyperglycemia, ketosis, acidosis
25
DKA Clinical Presentation
- Polyuria, polydipsia, weight loss
- Kussmaul respirations (compensatory)
- Fruity breath odor (acetone)

26
DKA Laboratory Findings
- Glucose typically 350-600 mg/dL
- Serum ketones positive at 1:2 dilution
- Anion gap >12 (often 20-30)

27
DKA Initial Management
- Fluids: 1-2L NS first hour
- Insulin drip at 0.1 unit/kg/hr
- K+ replacement when K+ <5.3
28
DKA Monitoring
- Check glucose hourly initially
- Monitor electrolytes q2-4h
- Transition to SC insulin when pH >7.3

29
DKA Complications
- Cerebral edema (pediatric cases)
- Hypokalemia from overcorrection
- Pre-renal AKI from dehydration
30
Toxicology Emergencies
- Consider in altered mental status
- Key toxidromes: anticholinergic, opioid
- Naloxone for respiratory depression

31
Anaphylaxis Management
- Epinephrine IM (0.3-0.5mg adults)
- Second-line: antihistamines, steroids
- Observe for biphasic reactions (20%)
32
Seizure Emergency Care
- Protect airway (recovery position)
- Benzodiazepines for active seizures
- Rule out reversible causes (e.g., hypoglycemia)
33
Sepsis Recognition
- SOFA score for organ dysfunction
- qSOFA: RR ≥22, SBP ≤100, AMS
- Time to antibiotics critical (hour-1 bundle)
34
Trauma Primary Survey
- ABCDE approach (Airway first)
- Control hemorrhage (tourniquets)
- C-spine immobilization if indicated
35
Pediatric Emergencies
- Different normal vital sign ranges
- Dehydration assessment (cap refill)
- Broselow tape for medication dosing

36
OB Emergencies
- Ectopic pregnancy rupture risk
- Pre-eclampsia (BP >140/90 + proteinuria)
- Postpartum hemorrhage management

37
Psychiatric Emergencies
- Suicide risk assessment (SAD PERSONS)
- Acute psychosis management
- Medical clearance before psych eval

38
Environmental Emergencies
- Heat stroke (core temp >40°C)
- Hypothermia (active rewarming)
- Drowning (ventilate even after prolonged submersion)

39
Key Highlights
- Important aspects of Emergency Conditions in Primary Healthcare
- Key points worth noting
- Considerations for the future

40
Conclusion & Key Takeaways
- Early recognition saves lives in emergencies
- Systematic approach to assessment
- Know when to refer to higher care

1 / 40